Submitted by CamilleBonta on
The North American Society for Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) and the Council of Pediatric Nutrition Professionals (CPNP) write in strong support of the inclusion of nutrition assessment data as a required data class in USCDI v7. Structured, interoperable nutrition assessment data are essential to patient safety, quality care, and equitable health outcomes across the lifespan.
NASPGHAN represents more than 3,000 pediatric subspecialist physicians caring for infants, children, and adolescents with gastrointestinal, hepatic, and pancreatic disorders—conditions in which nutrition assessment is fundamental to diagnosis, disease management, and therapeutic decision-making. CPNP represents about 350 pediatric nutrition professionals who perform and document nutrition assessments across inpatient, outpatient, and home-care settings.
![]()
Clinical and Patient Safety Rationale
Nutrition assessment is a comprehensive, systematic evaluation used to identify nutrition risk, deficiencies, and imbalances. Accurate, structured, and interoperable capture of core assessment elements - particularly anthropometric data—is foundational to identifying malnutrition, growth failure, and faltering weight across the lifespan. However, critical components of the nutrition assessment, including anthropometrics, food and nutrition history, current intake, nutrition-focused physical exam findings, and relevant biochemical and medical test data, are inconsistently structured, variably stored, and often unavailable across care settings within current EHR systems.
Key anthropometric elements — such as weight, height/length, occipito-frontal circumference (OFC), hand grip strength and z-scores for weight-for-height and BMI-for-age, mid-upper arm circumference (MUAC), and triceps skin-fold thickness — are required to operationalize established, evidence-based definitions of pediatric malnutrition and growth faltering. Without standardized and interoperable access to these data, clinicians are unable to reliably assess nutritional risk, track longitudinal growth patterns, or detect early deviations that warrant timely intervention.
Clear and structured documentation of nutrition assessment findings is essential to support downstream processes, including nutrition diagnosis, selection of appropriate nutrition interventions, and ongoing nutrition monitoring and evaluation. The assessment serves as the first critical step in the nutrition care process, enabling early identification of nutrition risk and informing personalized, evidence-based nutrition plans. When nutrition assessment data are incomplete, inaccessible, or fragmented, opportunities for prevention are missed—contributing to delayed interventions, prolonged hospitalizations, impaired recovery, increased mortality risk, and reduced quality of life.
The current fragmentation of nutrition assessment documentation disproportionately affects medically complex patienst, including infants and children transitioning across care environments, individuals with chronic disease, and populations experiencing food insecurity. These gaps contribute to inconsistent assessment, delayed diagnosis of malnutrition, and preventable patient harm. Improving the standardization and interoperability of nutrition assessment data within EHRs is therefore essential to enable continuity of care, support clinical decision-making, and advance patient safety and health outcomes across settings.
![]()
Public Health and Systems Impact
The lack of standardized, interoperable nutrition assessment data also undermines broader quality improvement, research, and public health surveillance efforts. Inconsistent documentation impairs the ability to:
- Apply standardized malnutrition definitions across institutions
- Identify system-level trends in growth faltering
- Evaluate effectiveness of nutrition interventions
- Support population health monitoring and equity initiatives
As faltering weight has recently been identified as an emerging pediatric safety and quality concern, interoperability of nutrition assessment data is necessary to move from identification to actionable, systemwide improvement.
![]()
Explicit Regulatory Requests for ONC (USCDI v7)
We respectfully request that ONC:
Include nutrition assessment as a required USCDI v7 data class
Require structured, interoperable representation of core anthropometric data, including:
Weight
Height/length
Occipito-frontal circumference (OFC)
Weight-for-height z-score
BMI-for-age z-score
Mid-upper arm circumference (MUAC)
Hand grip strength
Triceps skin fold
Ensure longitudinal interoperability of nutrition assessment data across:
Inpatient, outpatient, emergency, and home-care settings
Align USCDI nutrition assessment elements with established pediatric malnutrition and growth standards to support consistent diagnosis and clinical decision-making
USCDI v7 Alignment Map
| USCDI Priority Area | Nutrition Use Case | Safety Impact |
| Assessments | Nutrition status | Identifies at-risk, vulnerable patients for intervention |
| Care Transitions | Inpatient ↔ outpatient ↔ home infusion | Preserves nutrition assessment across settings |
![]()
Conclusion
Inclusion of structured, interoperable nutrition assessment data in USCDI v7 is essential to reducing preventable harm, enabling early identification of malnutrition and faltering weight, and ensuring continuity of care across settings. NASPGHAN and CPNP strongly urge ONC to prioritize nutrition assessment as a core clinical data element in USCDI v7.
Respectfully submitted,
NASPGHAN and CPNP
REFERENCE
Kersten, H. B., Goday, P. S., Abdelhadi, R., et al. (2026). Clinical practice guideline for diagnosis and management of faltering weight. Pediatrics, e2025075764. https://doi.org/10.1542/peds.2025-075764


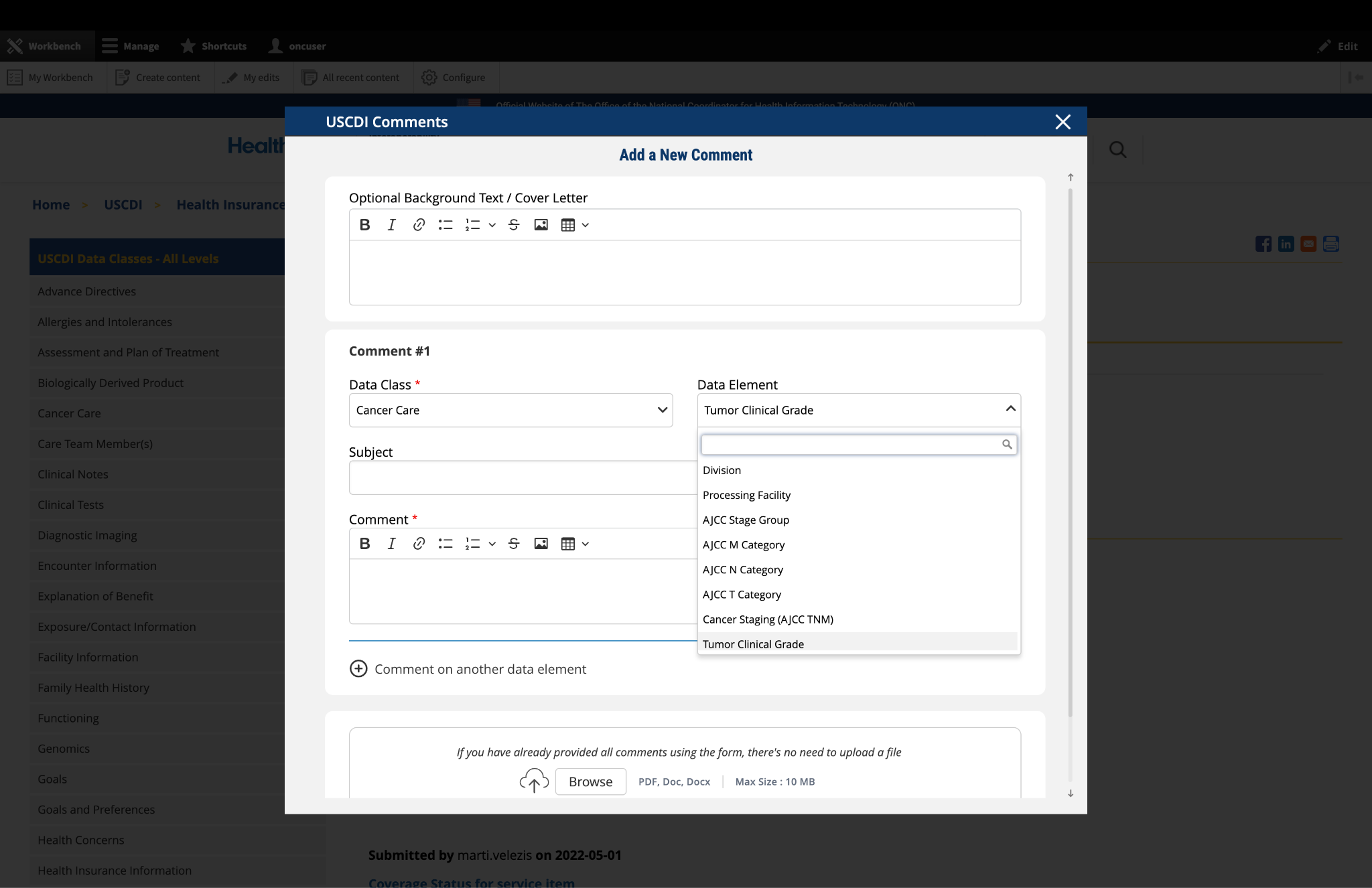
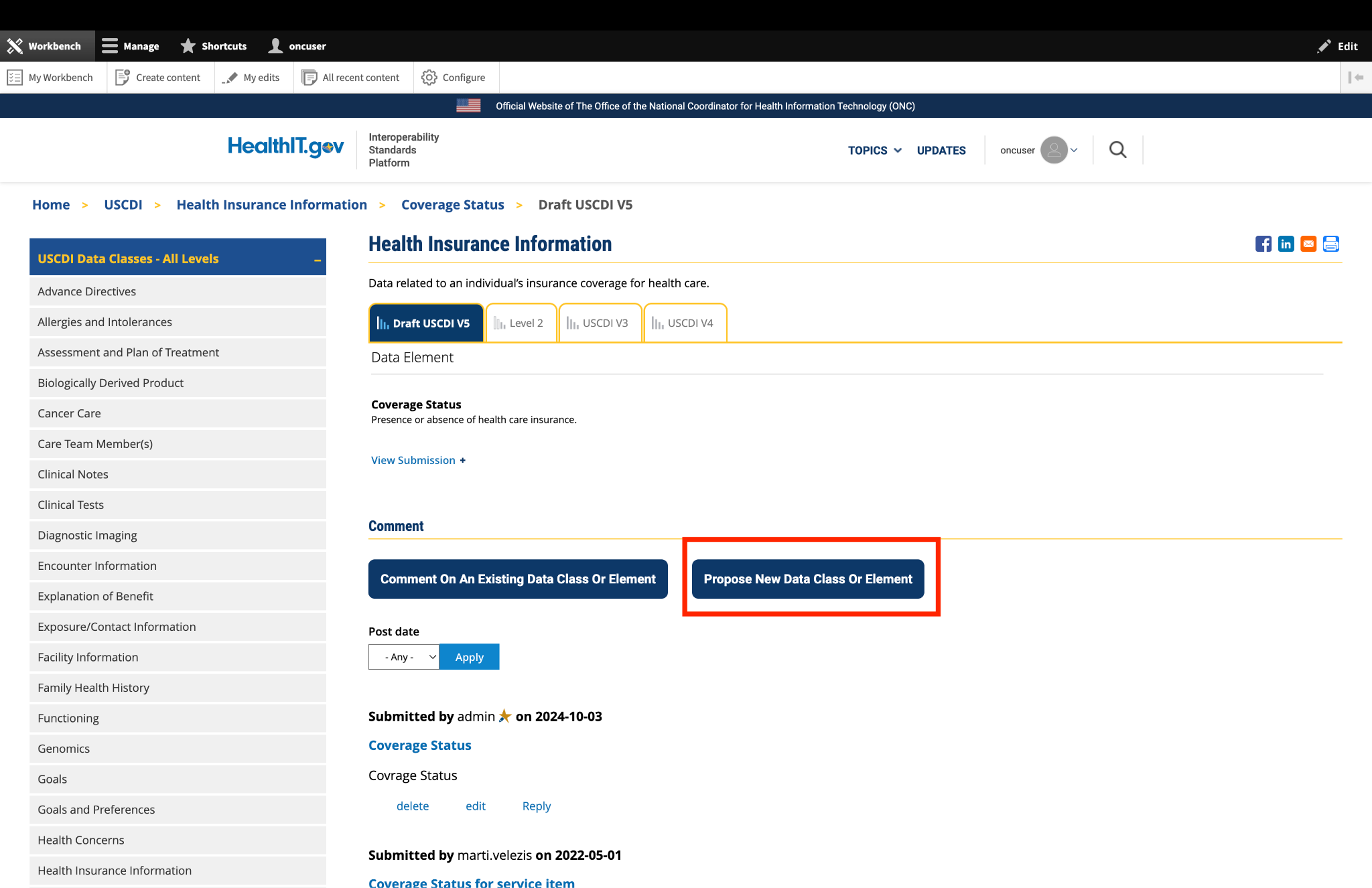
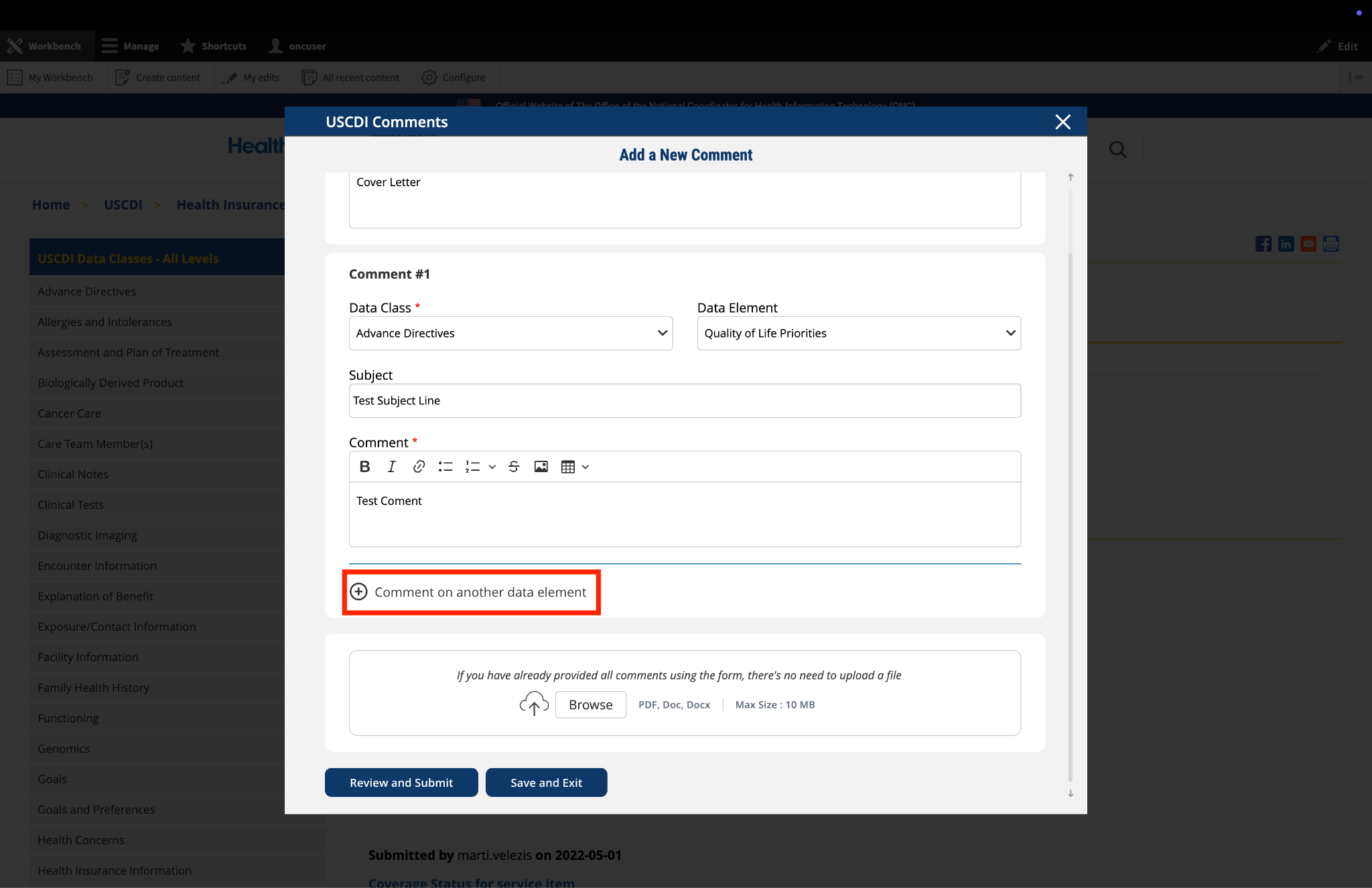
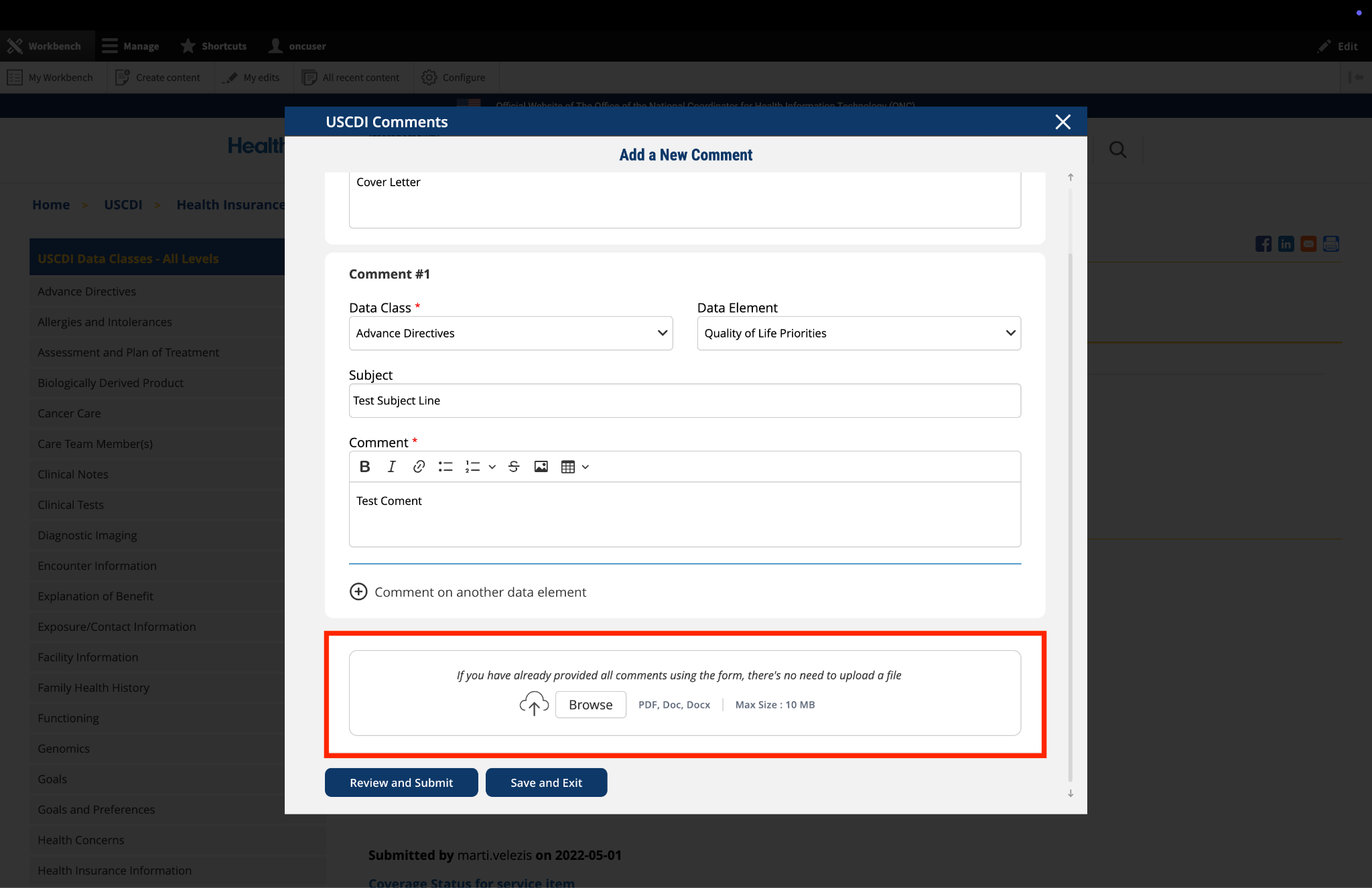
Submitted by jay.lyle@jpsys.com on
Nutrition Assessment insufficiently specific
USCDI says "Use of the USCDI standard is required as part of the new application programming interface (API) certification criterion". This suggests a certain level of specificity. Furthermore, the ONDEC guidelines are very clear that proposals include examples of collection, use, and exchange of this data element, with clearly defined scenarios, and that to achieve Level 1 or 2, submissions must answer yes to either vocabulary/terminology standardization or technical specification. This specificity is necessary, as the USCDI sets requirements that standards specifications must implement in a computably testable form.
None of this seems to be present for Nutrition Assessment. The term is ambiguous, as it could refer to the process of assessment (a procedure) or to the result of the assessment (a report or document, or perhaps just an observation). In AND terminology, the outcome is termed 'Nutrition Diagnosis,' which might suggest that the proposed element - not using the term 'diagnosis' - is intended to mean the process. The underlying request stipulates LOINC 75305-3, which sounds more like diagnosis.
No details are provided as to what either interpretation might consist of. Two supporting comments have been made with widely divergent assumptions, one suggesting that the assessment be composed of "weight, height/length, occipito-frontal circumference (OFC), hand grip strength and z-scores for weight-for-height and BMI-for-age, mid-upper arm circumference (MUAC), and triceps skin-fold thickness", the other of "underlying nutritional health including malnutrition risk, swallowing safety, self-feeding ability, and nutrient intake". AND lists a third set of requirements with some overlap but no clear correspondence.
If any data specification is to implement this requirement, there is no guidance that might support design decisions. The specification will necessarily be fundamentally vague, perhaps asserting a general LOINC code for nutrition assessment to be tagged onto an unstructured document, some instrument, or procedure, or any of the hundreds of data elements that might be germane.
Greater specificity would be helpful.