Submitted by ubackonja@mitre.org on
PACIO recommends advancing Transfer Summary Note to Level 2
Recommendation: Advance the Transfer Summary Note data element from Level 0 to Level 2.
Rationale: The PACIO Project Community* recommends advancing the Transfer Summary Note data element from Level 0 to Level 2. The Transfer Summary Note is a synopsis of a patient’s admission and clinical course in one setting that is generated to facilitate the patient being transferred to another setting. It is a foundational clinical document for ensuring safe, timely, and effective transitions of care between healthcare settings.
- Distinct importance of Transfer Summary Note vs. Discharge Summary: The Transfer Summary Note serves a distinct and time-critical function that is not addressed by the Discharge Summary Note. Transfer Summary Note must accompany the patient at the time of transfer to support patient safety and care decisions that must be immediately made at admission. In contrast, discharge summaries are often completed up to seven days after discharge and driven largely by billing and regulatory requirements. The content and timeliness of the Transfer Summary Note is essential for avoiding errors, providing appropriate care, and decreasing provider and patient burden; this note gives receiving providers needed immediate access to important patient information (e.g., C-CDA Transfer Summaryrequired patient information), such as their clinical status, active problems, current medications, allergies, recent procedures, and ongoing treatment plans to safely assume care without interruption.
Impact of transfer information in post-acute care (PAC): The distinction between Transfer Summary Note and Discharge Summary Note is particularly important for PAC settings, where patients are frequently transferred between hospitals, skilled nursing facilities, inpatient rehabilitation facilities, long-term acute care hospitals, and home health agencies. In these transitions, the absence of a standardized, timely transfer summary can lead to medication errors, missed diagnoses, duplicative testing, and preventable readmissions. The Transfer Summary Note helps avoid these issues by helping bridge the information gap that exists between the point of transfer and the eventual availability of a complete discharge summary.
Data Standard: The Transfer Summary Note data element is well represented by several established terminology and content standards.
- LOINC provides “Transfer summary note” code (18761-7).
- SNOMED-CT provides a “Transfer summary report (record artifact)” code (371535009).
The HL7® C-CDA (Consolidated Clinical Document Architecture) includes a dedicated Transfer Summary document template, most recently published in C-CDA Edition 4 (on FHIR®).
USCDI Level Criteria
Current Standards: Level 2 – Transfer Summary Note is represented by multiple terminology standards and SDO-balloted technical specifications.
- LOINC provides a “Transfer summary note” code (18761-7).
- SNOMED-CT provides a “Transfer summary report (record artifact)” code (371535009).
- The C-CDA on FHIR Implementation Guide (STU 1, v.1.2) provides a FHIR-based Transfer Summary profile on the Composition resource, enabling interoperability between CDA and FHIR implementations. The Transfer Summary template defines required, recommended, and additional sections for structured clinical content exchange and uses the document type code LOINC code 18761-7 for “Transfer Summary Note” as its required binding. C-CDA is one of the most widely implemented implementation guides for CDA and is used extensively for health information exchange across the United States.
The HL7 C-CDA v.2.0.0 (STU 2 Ballot) and C-CDA Edition 4 include a balloted Transfer Summary document template with defined required, recommended, and additional sections for structured clinical content.
Current Use: Level 2 – Transfer Summary Note data are captured, stored, or accessed in multiple production EHRs or other HIT modules from more than one developer.
- The C-CDA Transfer Summary template has been implemented in production EHR systems since its initial inclusion in C-CDA, supporting transitions of care documentation across healthcare organizations.
- Epic Systems supports the creation, storage, and retrieval of CCDA Documents through its FHIR R4 DocumentReference API. Epic’s publicly available FHIR APIs support interoperability with the comprehensive health record at clinics, hospitals, and health systems worldwide.
Oracle Health (Cerner) supports operation for querying document references, through its FHIR R4 APIs and Millennium platform.
Current Exchange: Level 2 – Transfer Summary Notes are electronically exchanged between production EHRs and HIT modules of different developers using available interoperability standards.
- Health information exchange networks, including those participating in eHealth Exchange, routinely exchange C-CDA documents including Transfer Summaries. The eHealth Exchange supports the exchange of billions of CDA documents annually across participating organizations.
- The US Government supports use of C-CDA to support health data exchange between different systems and providers, including C-CDA testing and support within its suite of ONC Certification tools.
Oracle Health Clinical Data Exchange uses C-CDA documents to deliver clinical event information including admit and discharge messages.
Breadth of Applicability: Level 2 – Use cases for Transfer Summary Note apply to most care settings.
- Transfer Summary Notes are used when patients move between acute care hospitals, emergency departments, skilled nursing facilities (SNFs), inpatient rehabilitation facilities (IRFs), long-term acute care hospitals (LTACHs), home health agencies, as well as hospice, home-based care, ambulatory care settings, behavioral health facilities, and medical transport between settings. These transitions are among the most clinically significant events in a patient’s care journey, as it is a particularly vulnerable time, that apply across virtually all care settings and specialties.
- The CMS Discharge Planning Final Regulation and the CMS Interoperability and Patient Access Final Rule require that all of a patient’s necessary medical information, including post-discharge goals of care and treatment preferences, must be documented and transferred along with the patient at the time of discharge to an appropriate receiving healthcare facility. The Transfer Summary Note serves as the standardized vehicle for this information exchange.
* The PACIO (Post-Acute Care Interoperability) Project, established February 2019, is a collaborative effort between industry, government, and other stakeholders, that aims to advance interoperable health information exchange between post-acute care (PAC) providers, patients, and other key stakeholders across health care.


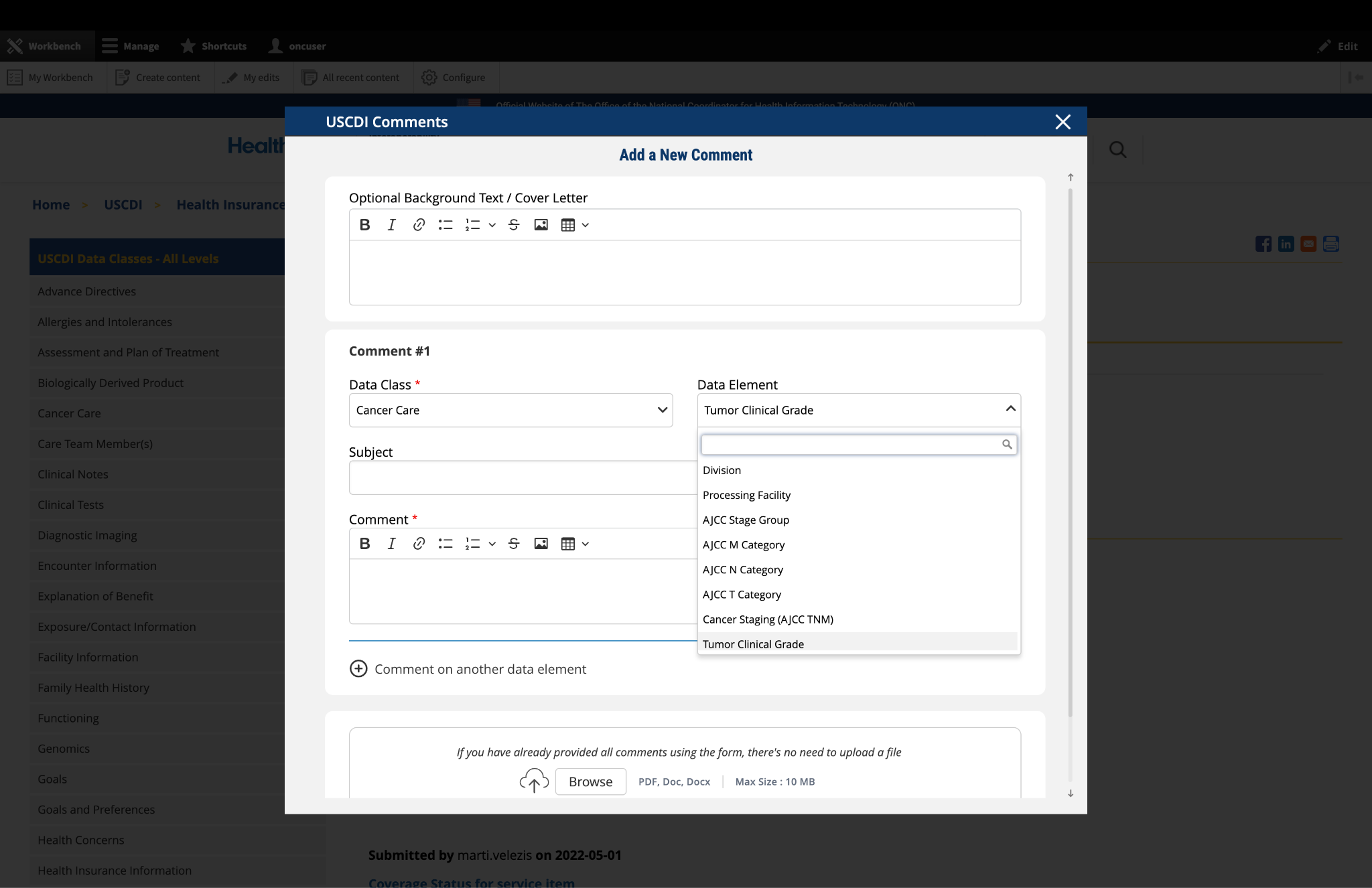
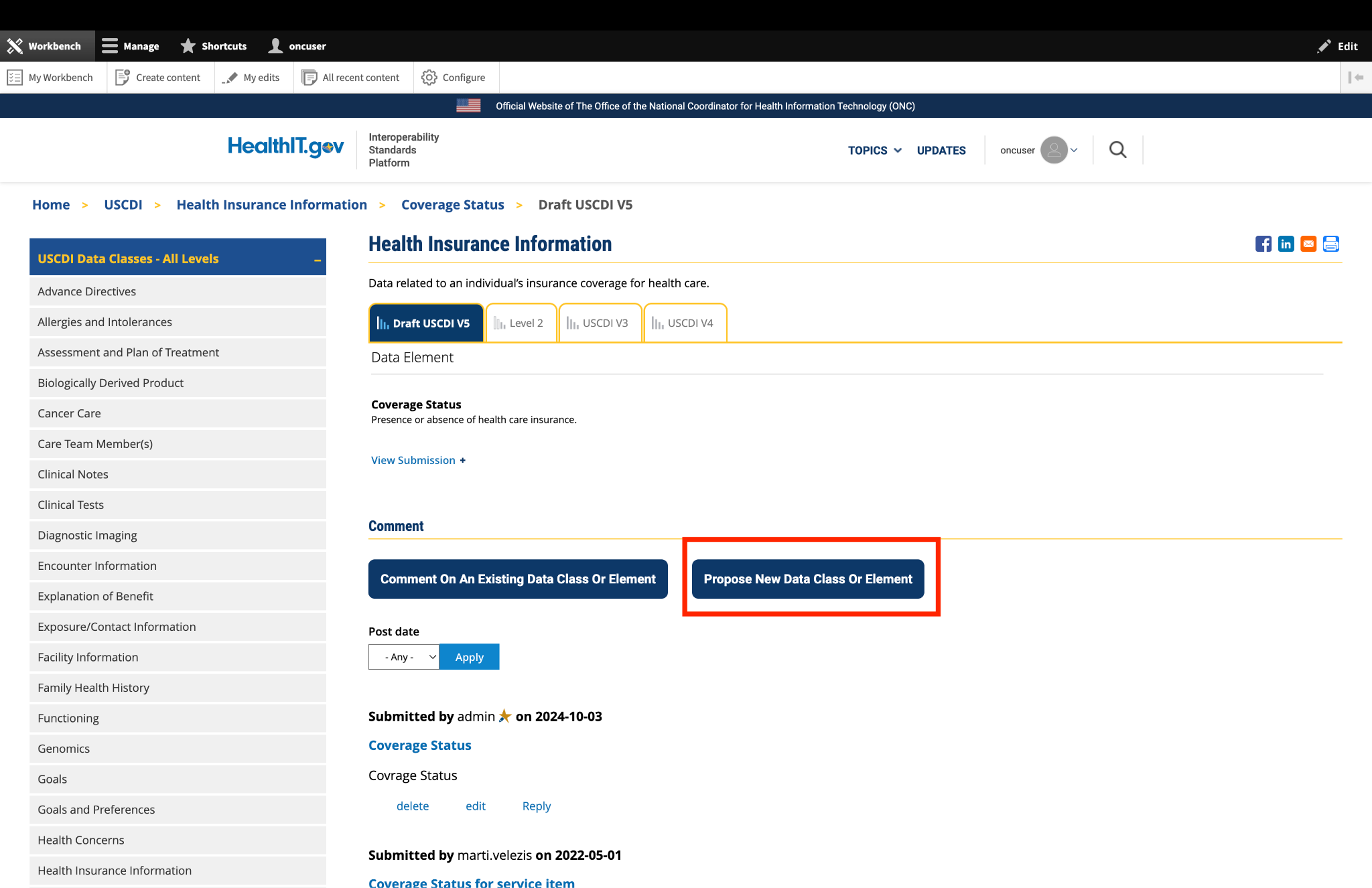
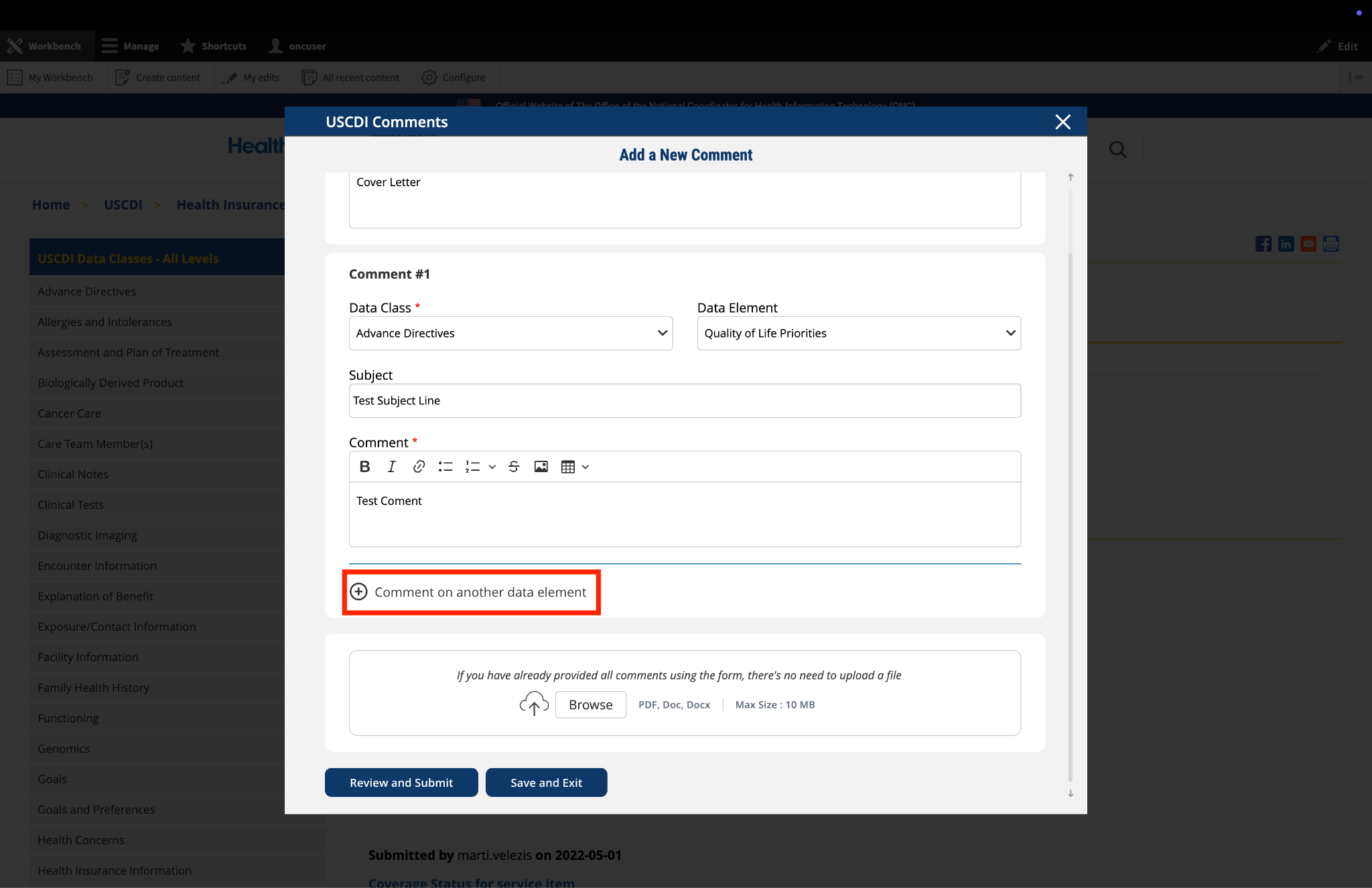
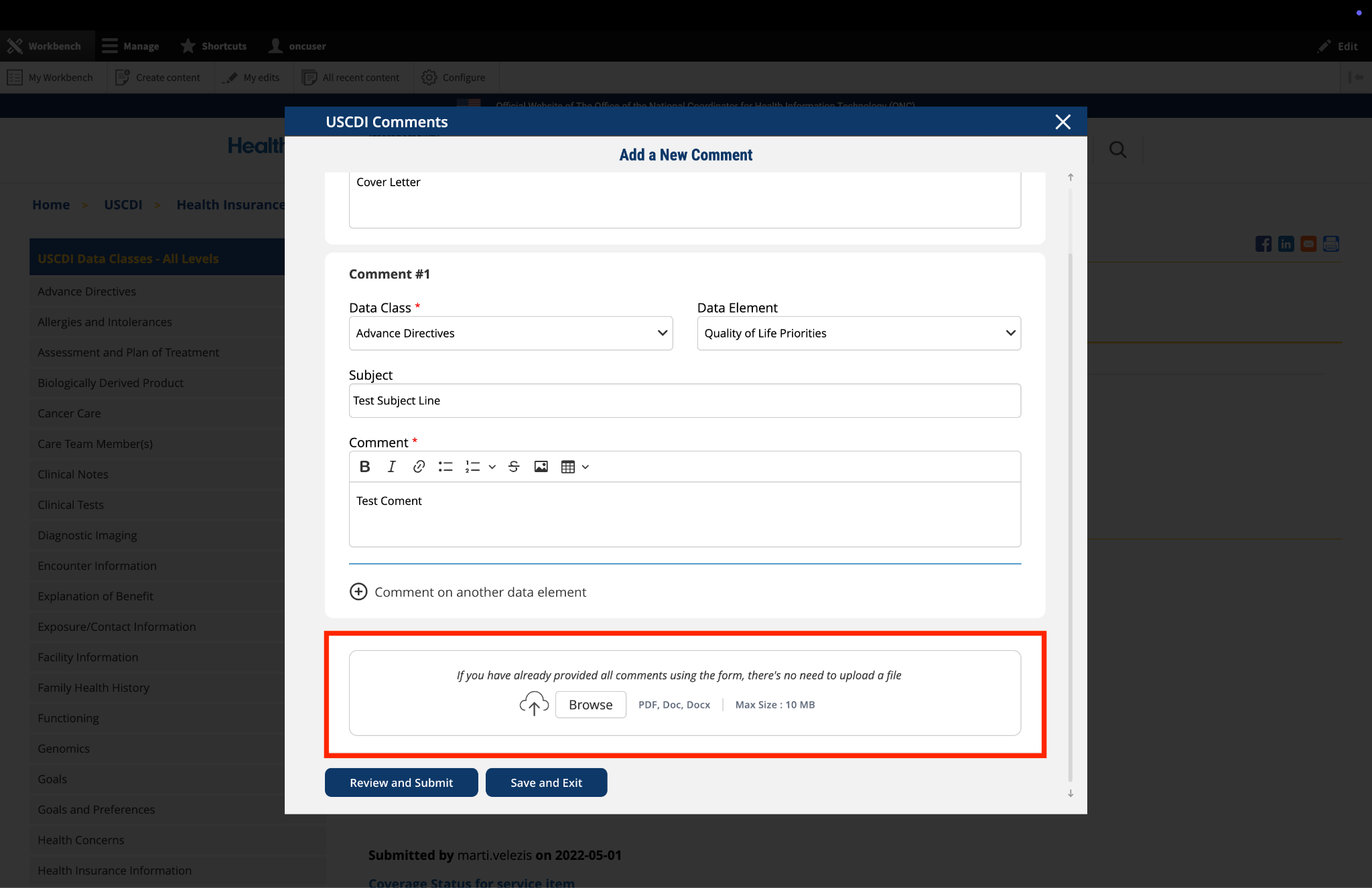
Submitted by NCQA on
NCQA Support for PACIO recommendation: Transfer Summary Note
NCQA supports the PACIO recommendation of advancing this element to Level 2, as a critical element for patient transfers and patient safety.