Submitted by BLampkins_CSTE on
Specimen Collection Method - CSTE Comment
| CSTE supports inclusion of Specimen Collection Method in USCDI v7. Collection of more granular laboratory data to support case adjudication and reporting as well as patient deduplication and linking of data from cases to ELR is critical for public health. The variables we recommend be added to USCDI v7 include: Name of testing/performing laboratory and associated identifiers (CLIA)(HIGH PRIORITY) Name of ordering provider and submitter Address of testing/performing laboratory Accession number at testing laboratory (HIGH PRIORITY for matching purposes) Date the test was ordered Date the test was performed (needs to be reconciled with results date/timestamp) Specimen collection date and time (HIGH PRIORITY) (Needs to be reconciled with Test Date=Clinically relevant time) Test result value (needs to be reconciled with values/results in USCDI V1 and V2), units, reference range and interpretation (HIGH PRIORITY) Abnormal flag (HIGH PRIORITY) Test kit identifier Dates and times are critical to evaluating the timeliness of reporting - it is a major indicator for the performance of public health surveillance systems and without this information it is unknown how data exchange is impacting the ability for public health to respond in a timely fashion. Although the date and time data are generated by the system, in practice it has been observed that availability of this data to Public Health Departments is sparse for use in timeliness analysis |


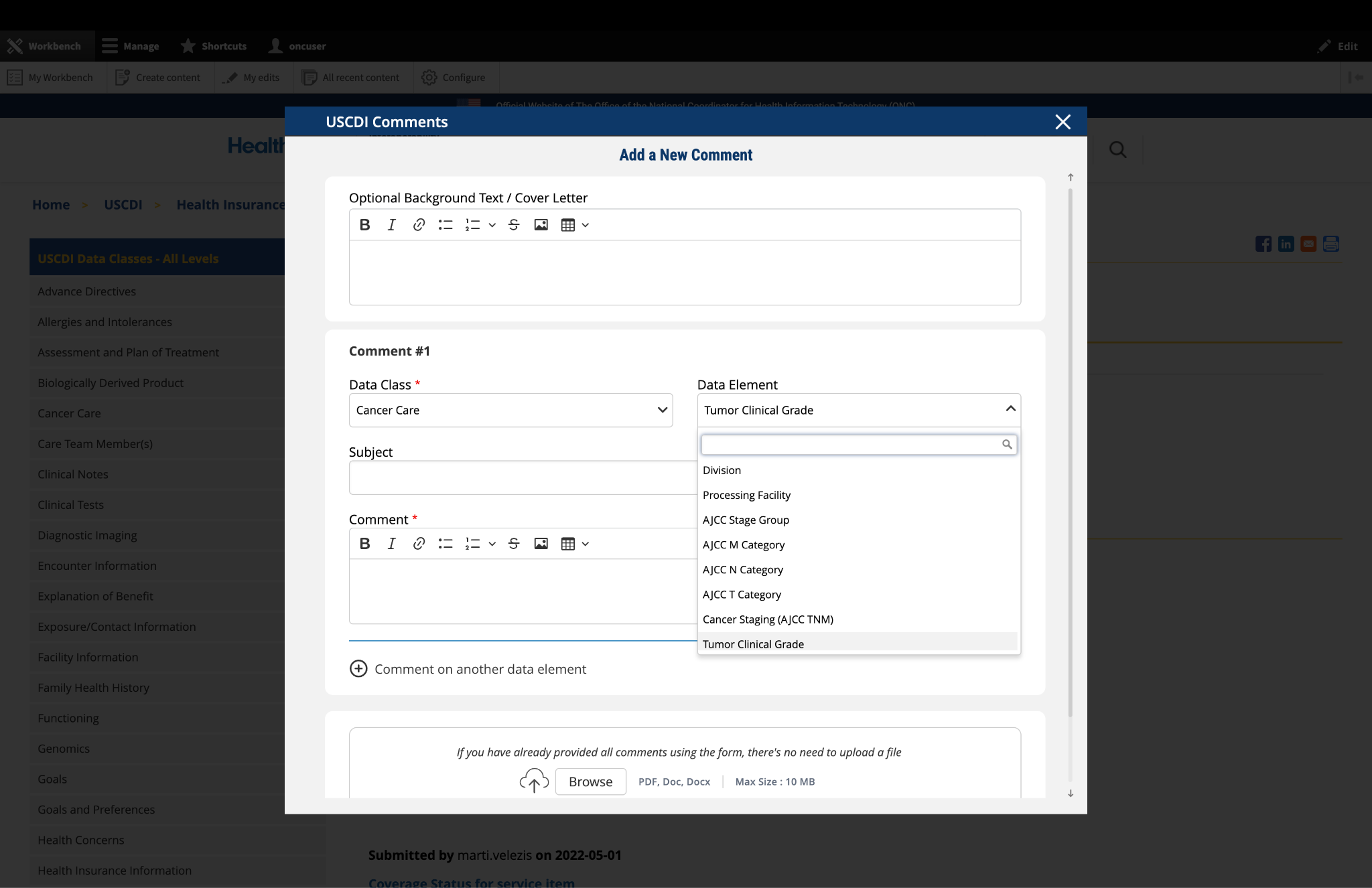
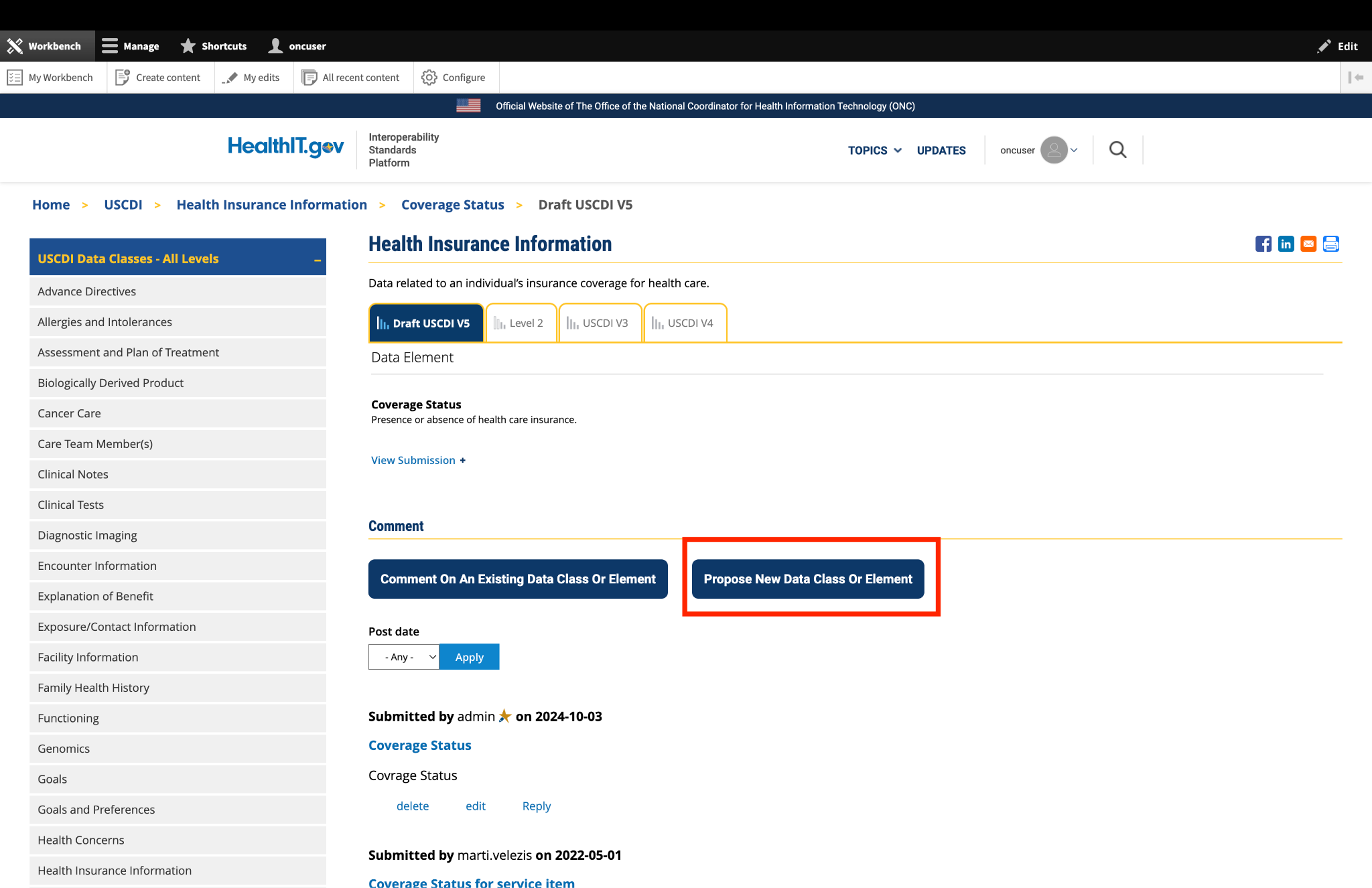
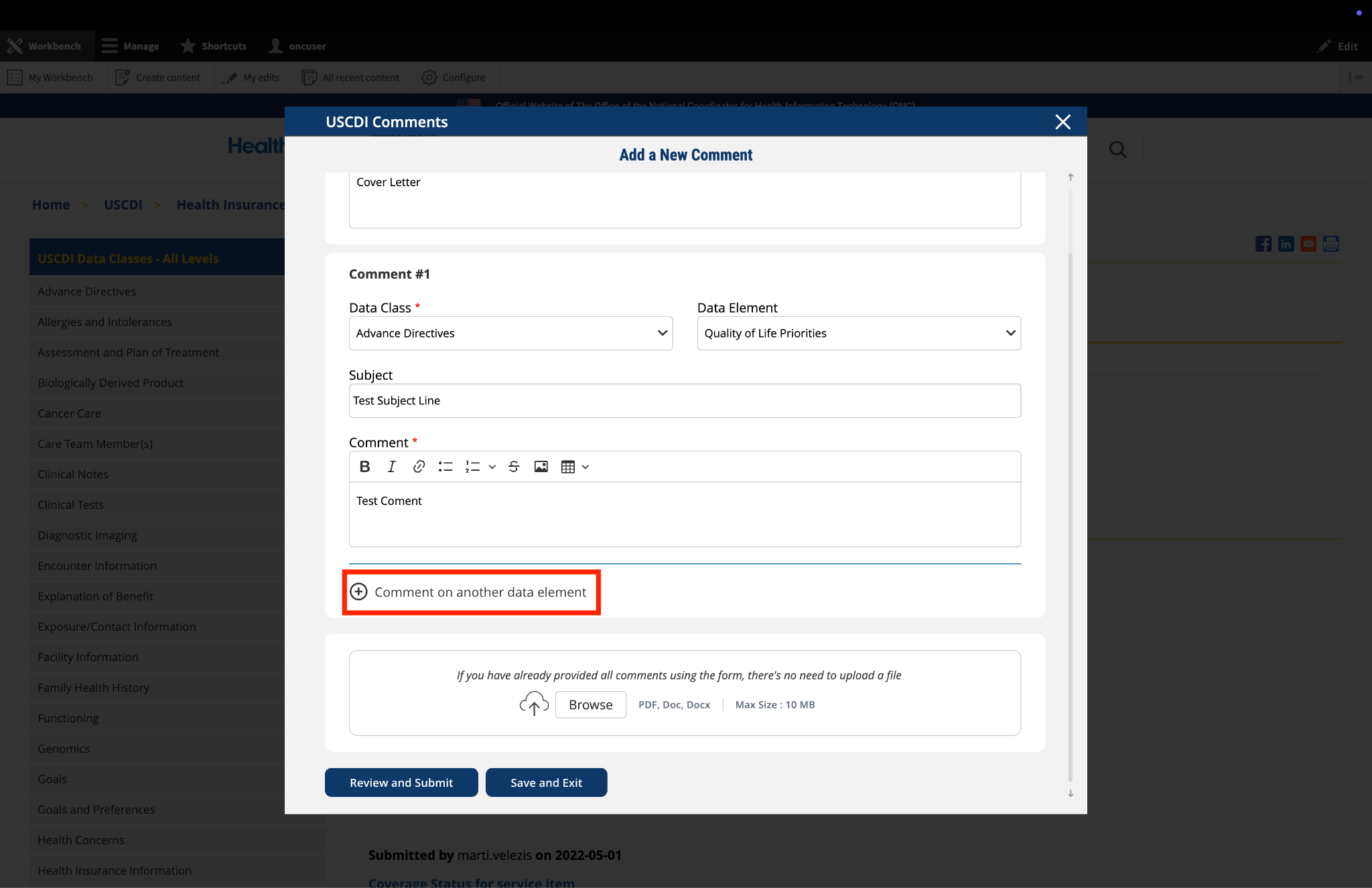
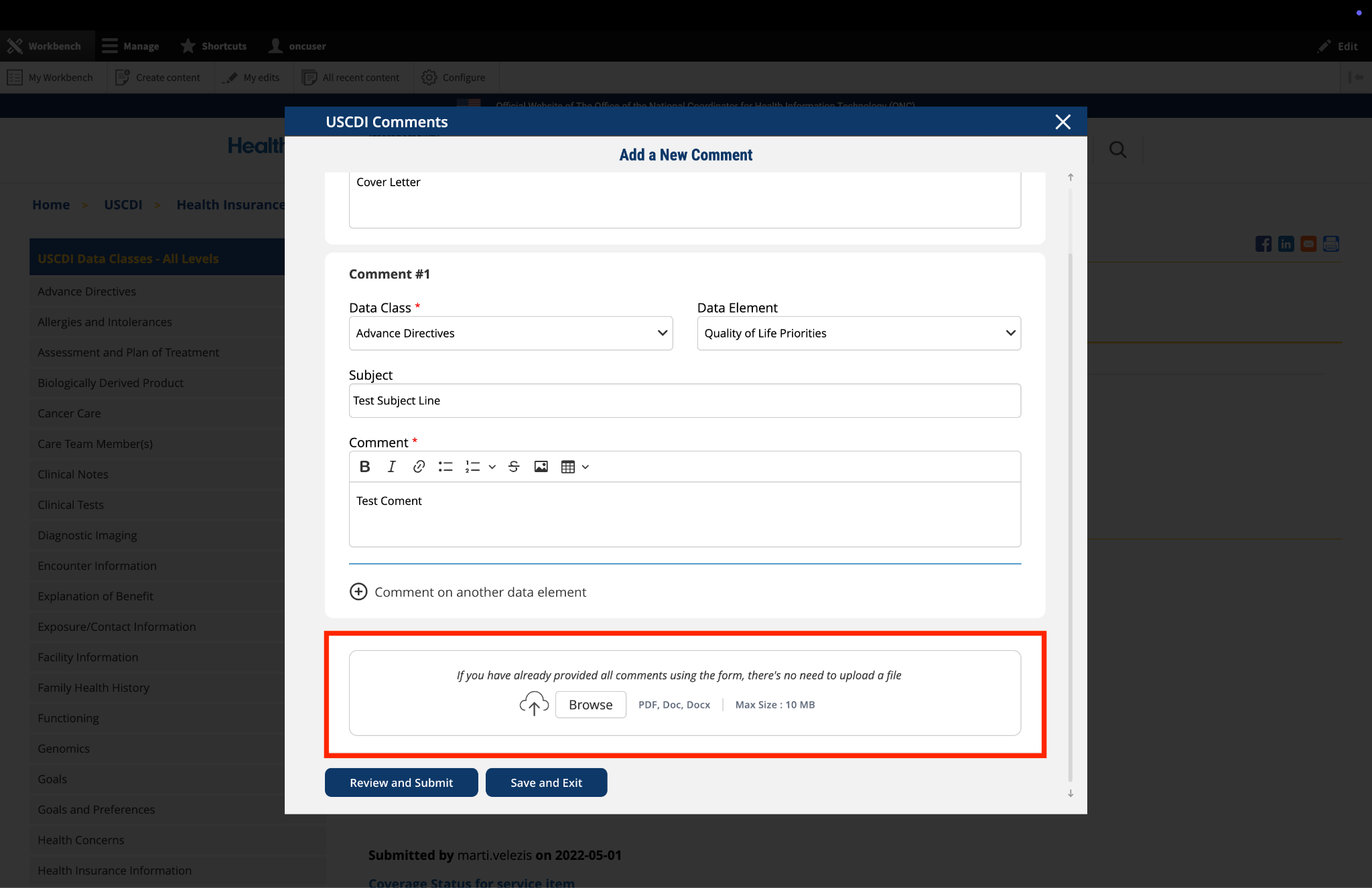
Submitted by jkegerize on
ACLA Comments: Specimen Collection Method
The American Clinical Laboratory Association (ACLA) appreciates the opportunity to comment on the Specimen Collection Method. Specimen Collection Method is not always received from the ordering provider and could be provided when available but not required. Certain collection methods can be presumed based on the ordered item. This data element is not supported in certified health IT. For example, blood tests are commonly obtained using venipuncture. This may add additional burden to the ordering provider.