| Submitted By: Joel Andress
/ Centers for Medicare and Medicaid Services (CMS) Center for Clinical Standards and Quality (CCSQ)
|
| Data Element Information |
| Data Element Description |
Devices are an identifiable grouping of mobility devices (i.e., wheelchairs), implantable devices (i.e., pace makers), or other wearable devices (i.e. compression socks or venous foot pump) with significant impact on patient functionality and health. The QDM v5.5 notes that “Device represents an instrument, apparatus, implement, machine, contrivance, implant, in-vitro reagent, or other similar or related article, including a component part or accessory, intended for use in the diagnosis, cure, mitigation, treatment, or prevention of disease and not dependent on being metabolized to achieve any of its primary intended purposes.” |
| Rationale for Separate Consideration |
USCDI v1 includes UDIs for implantable devices. We recommend expanding this to include data exchange for devices used, but external and implantable. |
| Use Case Description(s) |
| Use Case Description |
Device information, including devices applied/used is used extensively by hospitals, clinicians and providers submitting data for quality measurement. Device information is frequently used in quality measurement to identify frailty and advanced illness, but also used to identify health-care interventions for preventing, monitoring, or treating disease (i.e., an intermittent pneumatic compression device [IPC] for VTE prophylaxis or a cardiac pacemaker for heart failure).
The specific devices are currently reported as part of CMS quality measures:
• Frailty device indicators: wheelchair, walker, respiratory devices, continuous oxygen supply, identifier of confined to bed/chair
• Cardiac pacers
• Wearable devices: Graduated Compression socks, Intermittent pneumatic compression, venous foot pump
|
| Estimate the breadth of applicability of the use case(s) for this data element
|
More than 4,000 hospitals and 1 million providers currently capture, access and exchange this device information. This information is currently electronically submitted by providers and hospitals to CMS for quality measurement.
eCQI resource center, includes measure specifications for CMS program eCQMs (i.e. CMS 190, CMS 125): https://ecqi.healthit.gov/ecqms |
| Link to use case project page |
https://ecqi.healthit.gov/ecqms |
| Use Case Description |
Data exchange of device information is also critical for clinical care. Clinician’s need to be aware of prior and recent healthcare interventions and the presence of implanted devices or use of external or mobility devices for optimal patient health-care provision. |
| Estimate the breadth of applicability of the use case(s) for this data element
|
Majority of hospitals and clinicians caring for patients should be capturing and exchanging this information. |
| Healthcare Aims |
- Improving patient experience of care (quality and/or satisfaction)
- Improving the health of populations
- Improving provider experience of care
|
| Maturity of Use and Technical Specifications for Data Element |
| Applicable Standard(s) |
SNOMED CT (Frailty Device, value set OID: 2.16.840.1.113883.3.464.1003.118.12.1300)
SNOMED CT (Intermittent Pneumatic Compression Devices (IPC), value set OID: 2.16.840.1.113883.3.117.1.7.1.214)
SNOMED CT (Graduated Compression Stockings (GSC), value set OID: 2.16.840.1.113883.3.117.1.7.1.256)
SNOMED CT (Venous Foot Pumps (VFP), value set OID: 2.16.840.1.113883.3.117.1.7.1.230)
SNOMED CT (Cardiac Pacer, value set OID: 2.16.840.1.113883.3.526.3.1193)
ICD-10-CM, SNOMED CT (Cardiac Pacer in Situ, value set OID: 2.16.840.1.113883.3.526.3.368)
https://vsac.nlm.nih.gov/valueset/expansions?pr=ecqm
|
| Additional Specifications |
HL7 FHIR US Core Implementation Guide STU3 based on FHIR R4, Implantable device profile, already required by USCDI v1 to specify device UUID
(https://www.hl7.org/fhir/us/core/StructureDefinition-us-core-implantable-device.html)
HL7 FHIR QI Core Implementation Guide STU4 based on FHIR R4, Device and DeviceUseStatement profiles.
(http://hl7.org/fhir/us/qicore/StructureDefinition-qicore-device.html , http://hl7.org/fhir/us/qicore/StructureDefinition-qicore-deviceusestatement.html )
CMS Quality Data Model (QDM) version 5.5 Guidance (https://ecqi.healthit.gov/sites/default/files/QDM-v5.5-Guidance-Update-May-2020-508.pdf)
HL7 C-CDA Release 2.0, Unique Device Identifier (UDI) for Implantable Medical Devices (http://www.hl7.org/implement/standards/product_brief.cfm?product_id=486)
|
| Current Use |
Extensively used in production environments |
| Supporting Artifacts |
Device use data is routinely captured in EHR systems used by hospitals and providers, particularly for quality measurement purposes.
https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/MMS/Quality-Programs
https://ecqi.healthit.gov/ecqms
https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/MMS/Quality-Programs
|
| Extent of exchange
|
5 or more. This data element has been tested at scale between multiple different production environments to support the majority of anticipated stakeholders. |
| Supporting Artifacts |
Device information data for quality measurement is electronically exchanged from an organization’s EHR system to CMS for reporting and payment quality measurement programs, via QRDA files and other architectures. These device data elements have been tested for reliability and validity of capture during the development of CMS eCQMs and can be feasibly captured and exchanged. Ongoing testing for exchanging these data in FHIR standards via HL7 Connectathons.
ONC also requires the availability and exchange of implantable device UIDs, which can be broadened to include the devices used by a patient.
https://ecqi.healthit.gov/qrda
https://www.healthit.gov/test-method/implantable-device-list
https://confluence.hl7.org/display/FHIR/2020-09+Clinical+Reasoning
https://ecqi.healthit.gov/qrda
|
| Potential Challenges |
| Restrictions on Standardization (e.g. proprietary code) |
No challenges anticipated. This data is available in standard terminology that can be publicly access via the VSAC and HL7. |
| Restrictions on Use (e.g. licensing, user fees) |
We are not aware of any restrictions. |
| Privacy and Security Concerns |
This data, like any patient data should be exchanged securely. Current processes exist, governed by CMS and ONC, to securely transfer this data element. |
| Estimate of Overall Burden |
Device data is regularly captured by a broad range of healthcare providers, and should not cause excess burden to implement. Some burden may be required to expand the QI Core profiles available for this information to US Core. |
| Other Implementation Challenges |
N/A |


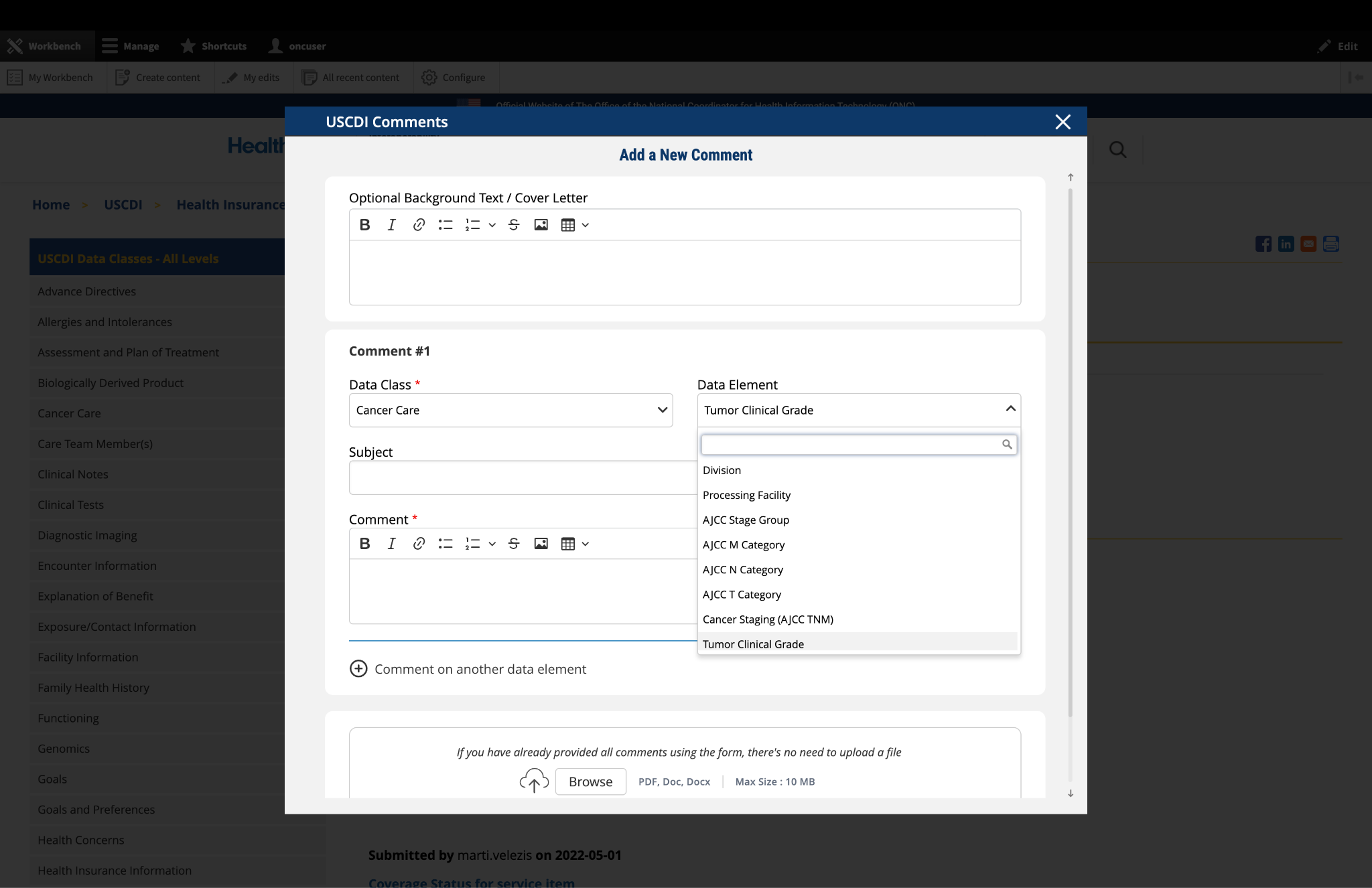
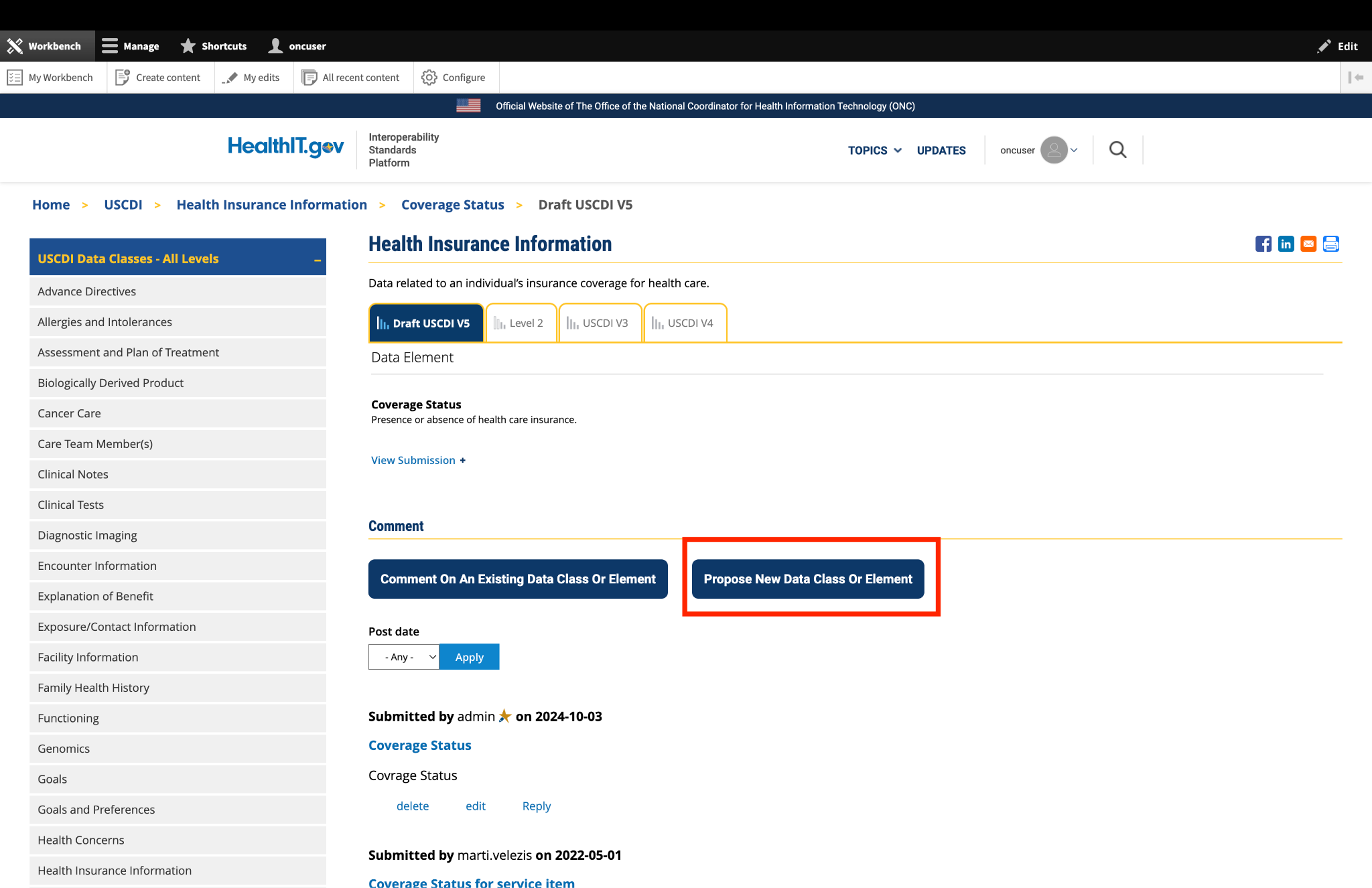
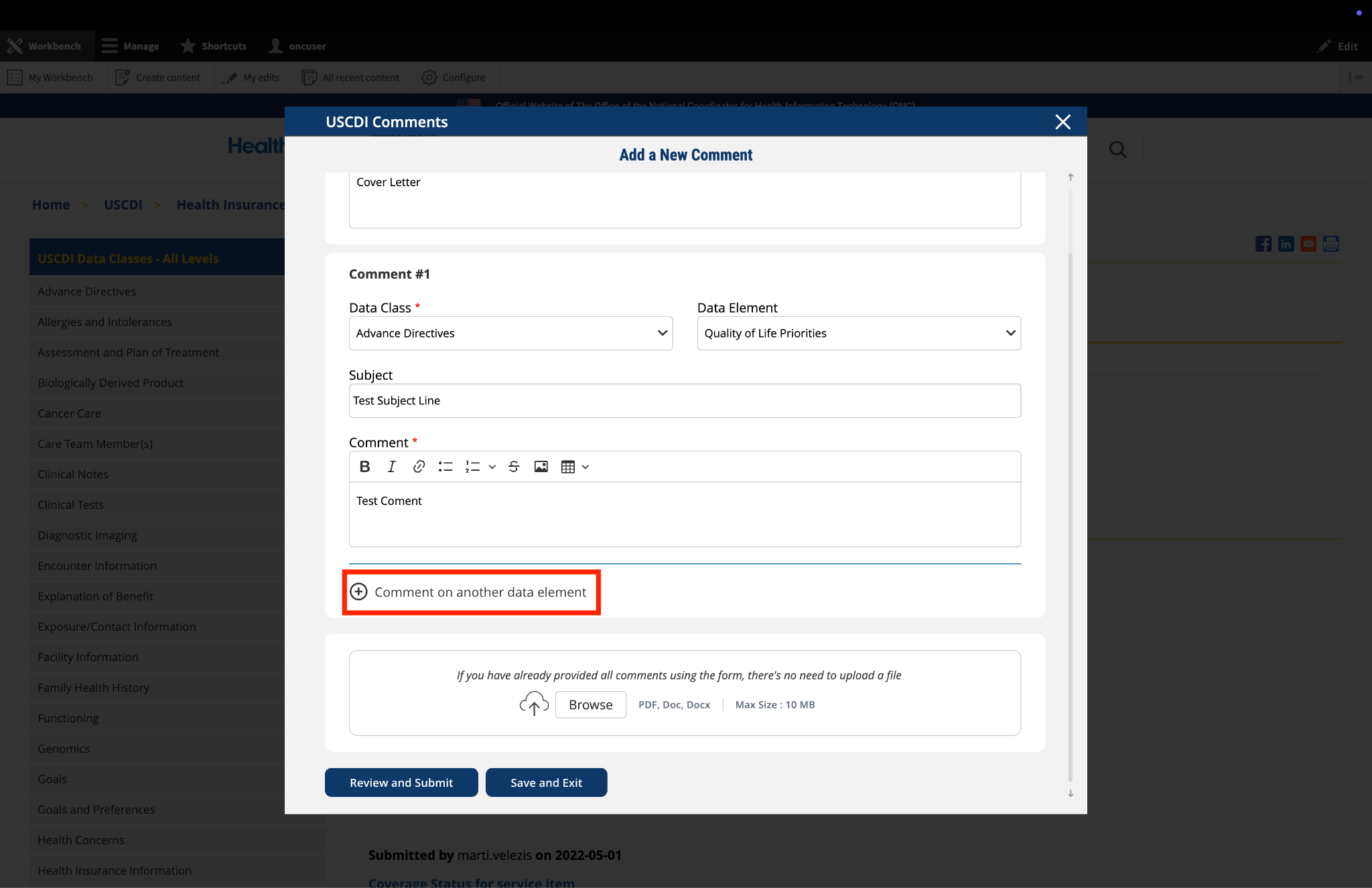
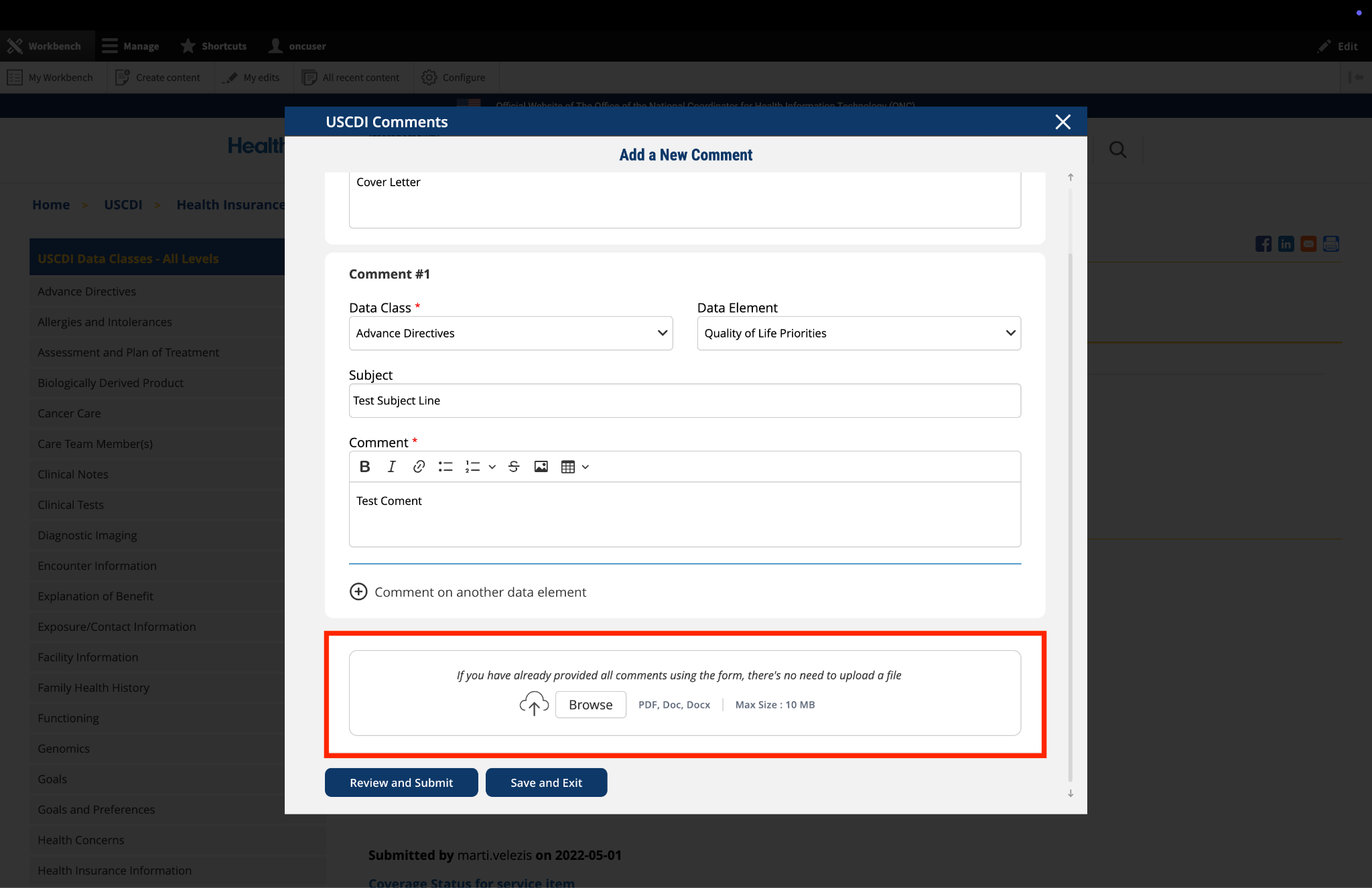
Submitted by EmoryHealthcare on
Emory Healthcare comments on Device Type
EHC appreciates the need to and utility of specifying device types, but we have concerns about the ambiguity of certain devices. For example, an intrauterine device is considered both a medical device and a medication. We seek clarity from ONC on how devices like those might be best documented.