Submitted by ubackonja@mitre.org on
PACIO supports NCQA’s Health Status Assessment recommendation
The PACIO Community support’s NCQA’s recommendation to clarify the scope of the Health Status Assessment data class to include both the assessment and the result or answer of that assessment because it complements existing data capture and transmission practices that are required in post-acute care (PAC) settings. In order to receive Medicare reimbursement from CMS, PAC facilities are required to complete specific standardized assessments, the results of which are reported to CMS as mandated by Congress. NCQA’s recommendation to include the results along with the assessment would facilitate the capture and transmission of these required data, supporting care quality for patients and fiscal stewardship for the Medicare program. Therefore, the PACIO community support’s NCQA’s recommendation as it complements existing workflows and supports quality care.


Submitted by NCQA on
NCQA recommendation: Health Status Assessment clarification
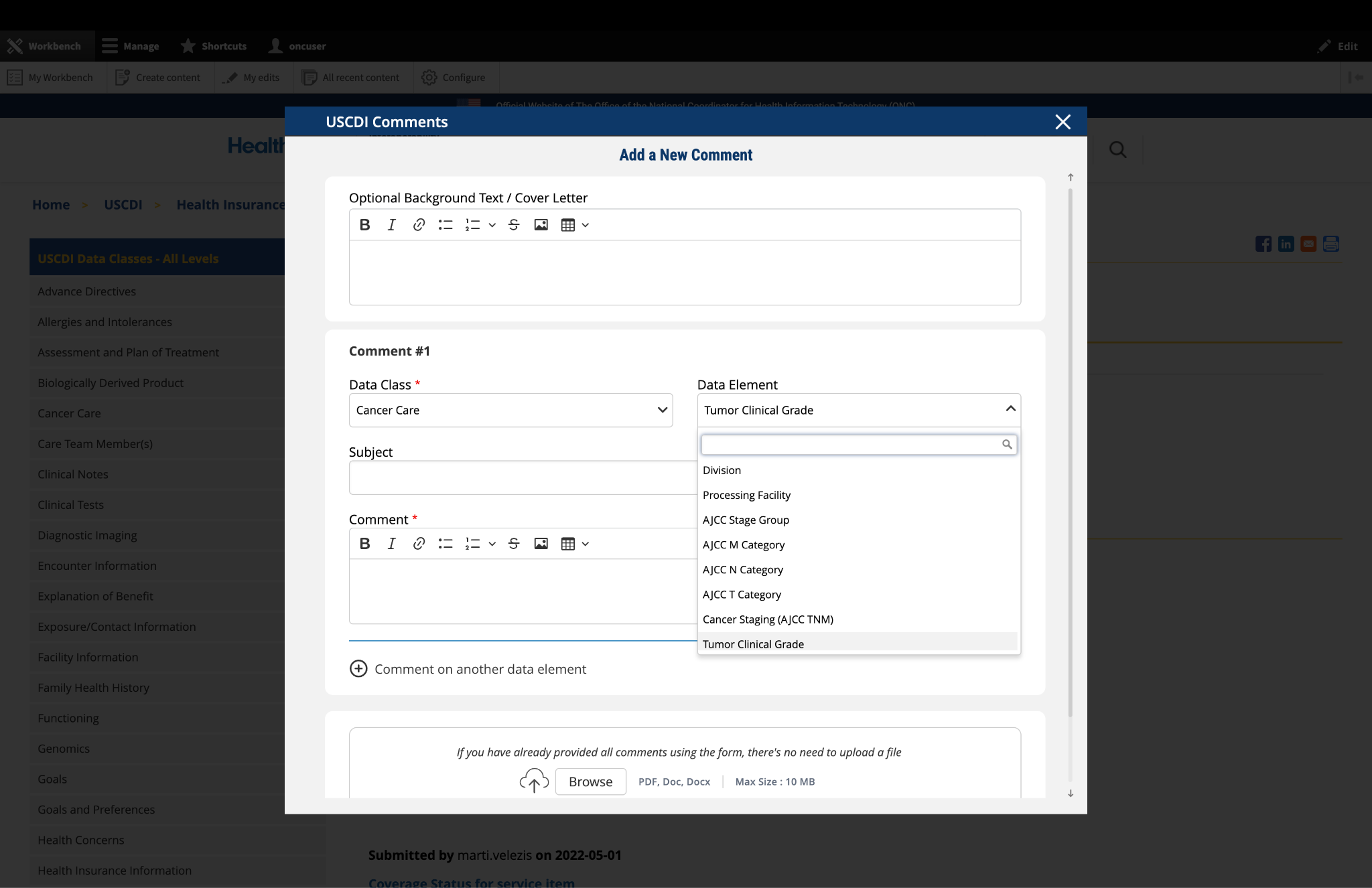
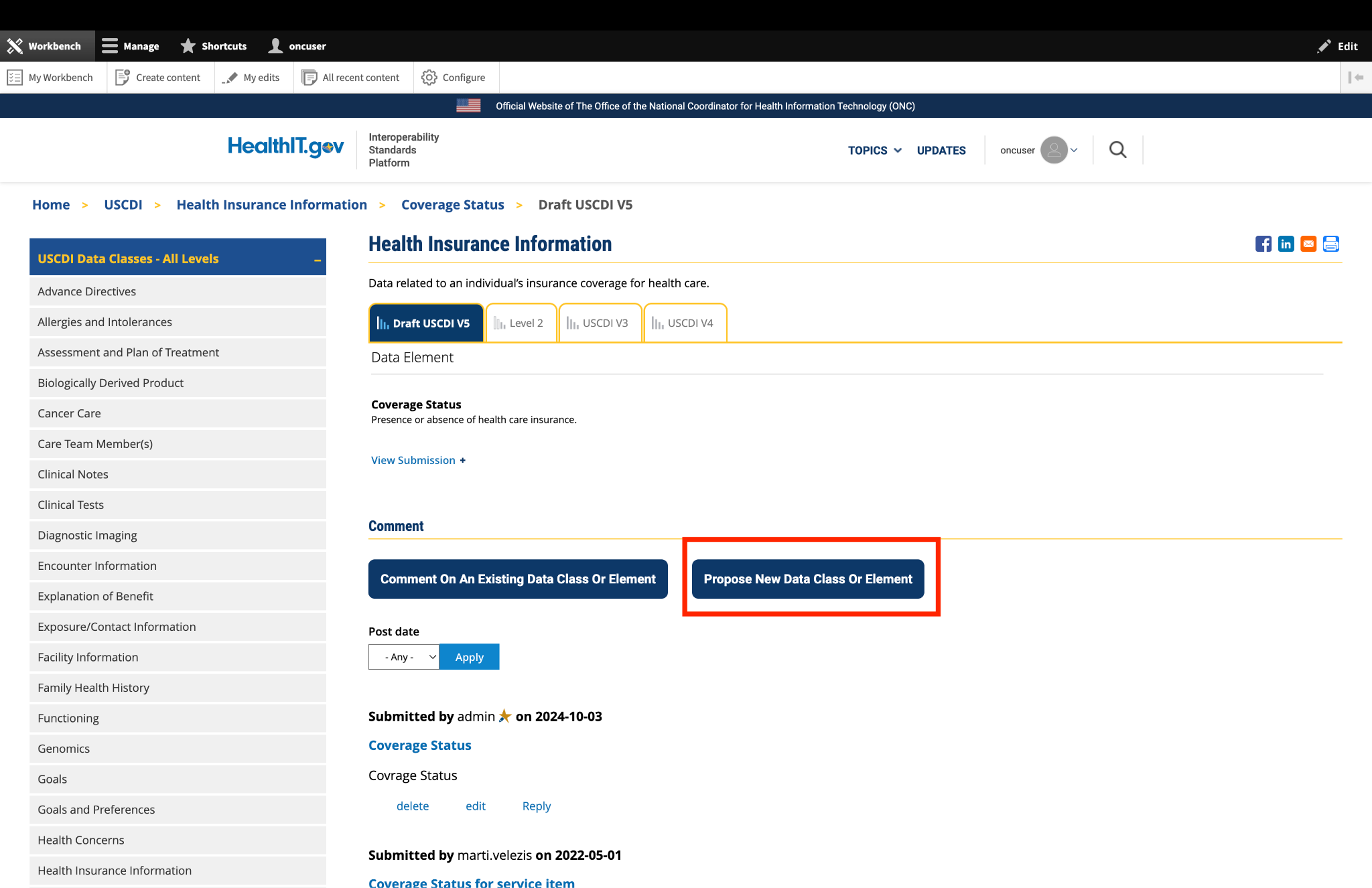
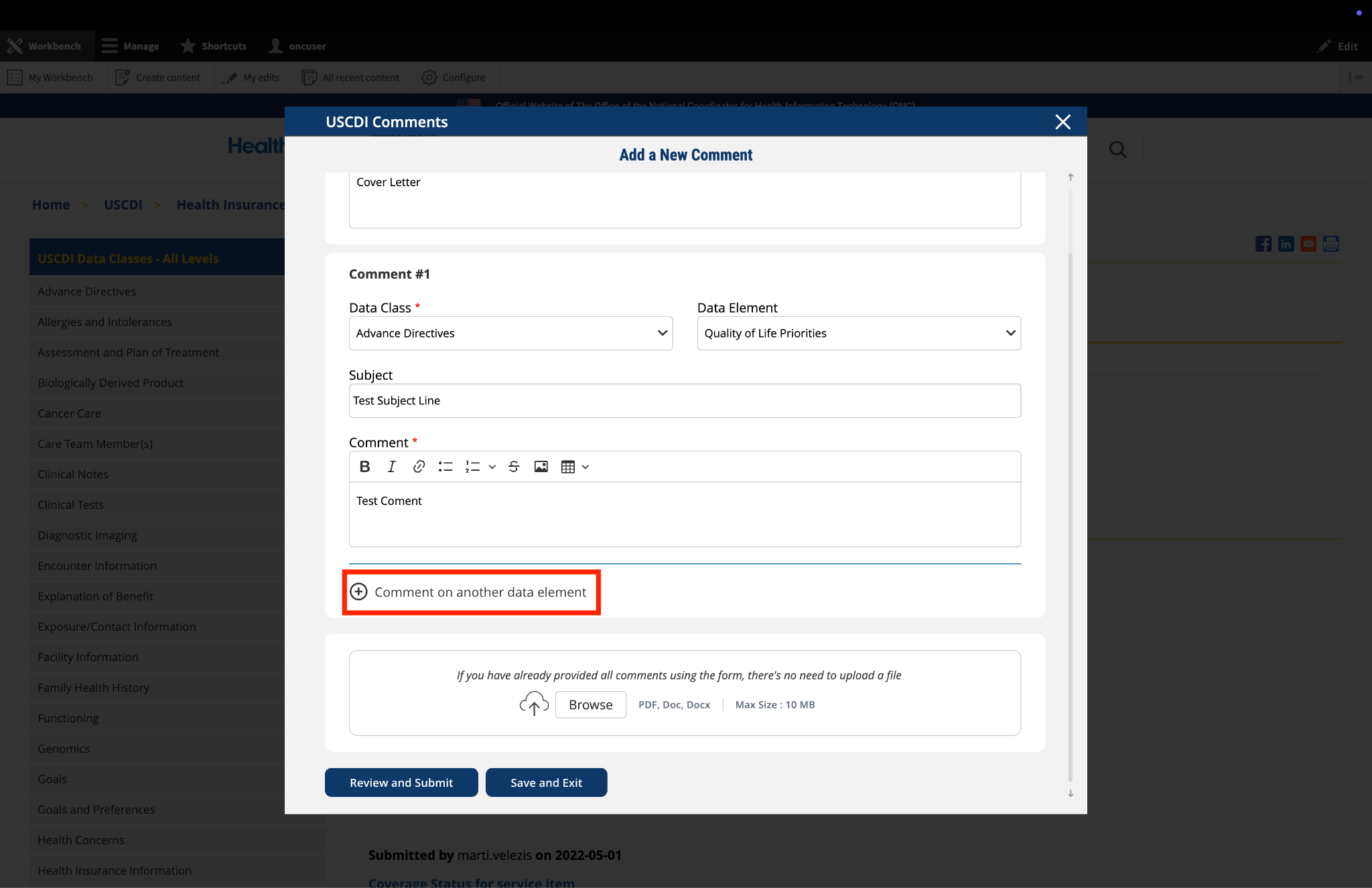
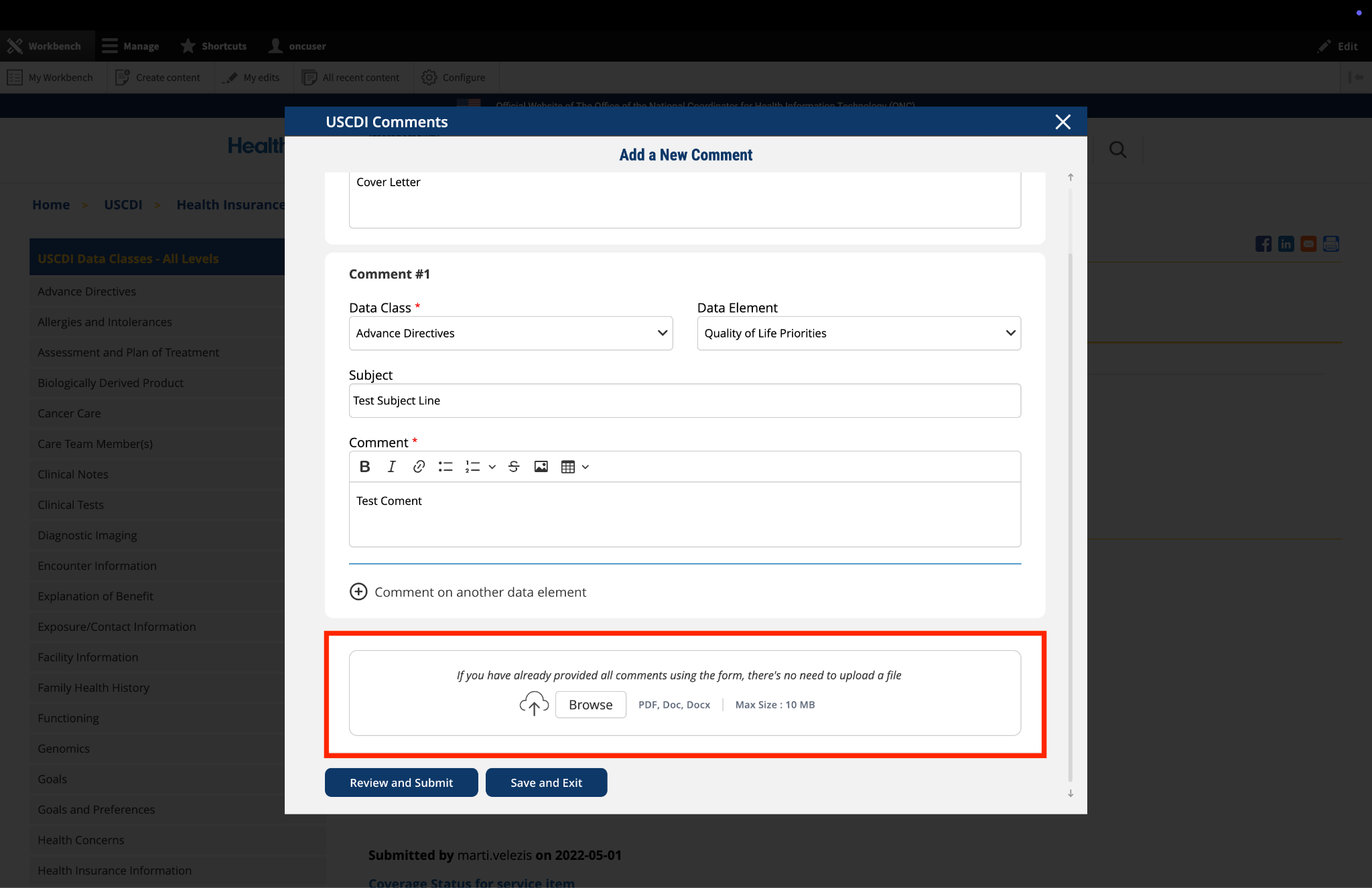
Recommendation: Clarify the scope of the Health Status Assessment data class to include both the assessment (LOINC) and the result or answer of that assessment (often LOINC answer codes, SNOMED CT, or quantitative result).
o Update the data class definition: Assessments and results of a health-related matter of interest, importance, or worry to a patient, patient’s authorized representative, or patient’s healthcare provider that could identify a need, follow-up care or a condition.
o Update the individual element definitions to include the assessment and result as well as LOINC and SNOMED for applicable vocabulary.
Example: Tobacco Use: Assessment and result of a patient’s tobacco product use behaviors. Applicable Vocabulary: LOINC, SNOMED CT
Example: Mental/Cognitive Status: Assessment or screening and result for the presence of a mental or behavioral problem. Applicable Vocabulary: LOINC, SNOMED CT
Rationale: In patient care and quality measurement, knowing that both the assessment occurred and the result of that assessment is critical for care decisions and determining any additional testing, diagnoses, procedures or interventions (i.e., education) that may be required. The completion of a health status assessment does not always result directly in a diagnosis or procedure represented by other USCDI/USCDI+ data elements, but instead the result of health status assessments are used in conjunction with other data related to the patient to guide care. The clarification of scope of this data class will support consistent implementation and exchange of critical data for patient care. Additionally, applying this recommendation would align to the setup of other data classes, including Clinical Tests, Diagnostic Imaging and Laboratory. In NCQA’s HEDIS, we assess both that a specific assessment/screening was completed (i.e. tobacco use or depression screening) and that a result of the assessment/screening is present. The result is often used to assess for appropriate follow-up, which may include rescreening, counseling, or other follow-up interventions.